
It is surprising that the wellness industry hasn’t paid more attention to endocrine disruptors—a “silent killer” of wellbeing for humans and the planet. Endocrine disruptors (and more specifically EDCs—Endocrine Disrupting Chemicals) are linked to numerous adverse health outcomes such as alterations in sperm quality and fertility, abnormalities in sex organs, early puberty, altered nervous system function and immune function, certain cancers, and respiratory problems—both in humans and wildlife.
However, the existence of only a very limited number of specific endocrine disruptors has been proven. The reason being that exposure to them is manifold and difficult to control, and the biological consequences remain poorly understood and complex to study because the effect of the toxicity is often long-term, not immediate.
Yet, endocrine disruptors are both diverse and widespread, with humans and animals alike frequently exposed to numerous sources of contamination. They can be found in manufactured goods as well as plant or animal-based foods, with most originating from the agrochemical industry (pesticides, plastics, pharmaceuticals, etc.) and its waste products. Many are residual: They persist in the environment for years and years, and they may be transferred between soil, water and air many years after their initial production.
But recently (since 2016), there has been major scientific progress, with about 15 probable “exposure-outcome” associations identified and a much deeper understanding of the effects of EDCs on human health. Evidence is now almost incontrovertible (“particularly strong” in the prudent language of science) for relations between perfluoroalkyl substances (used in an ever-expanding group of manufactured chemicals found in everyday products ranging from carpets resistant to stains to anti-sticking cookware) and child and adult obesity, impaired glucose tolerance, gestational diabetes, reduced birth weight, reduced semen quality, polycystic ovarian syndrome, endometriosis, and breast cancer.
Similarly, strong evidence exists for associations between bisphenols and adult diabetes, reduced semen quality, polycystic ovarian syndrome, and attention-deficit disorder in children following prenatal exposure.
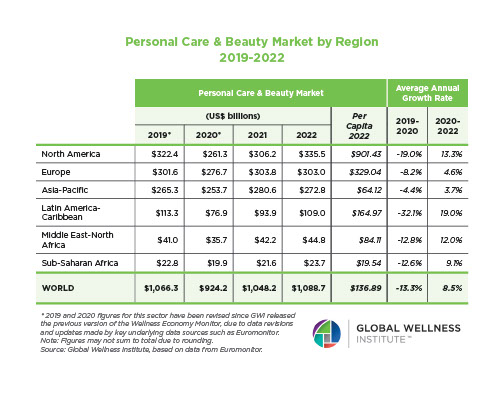
The list goes on—adding to the growing evidence that exposure to EDCs should be reduced through regulatory action for the sake of mental and physical health and wellbeing. Some countries and regions have made progress, but others lag behind. In the US, for example, the so-called Kehoe rule stipulates that suspicious chemicals should be assumed innocent until proven guilty—explaining why the country kept lead in petrol for more than five decades after its danger was first suspected and why the US government has so far banned only 11 substances in cosmetics/beauty products.
By contrast, in the EU—which gives human safety precedence over chemicals when strongly in doubt about their effects and associations—more than one thousand substances have so far been banned in beauty products.
In light of all the above and from a wellness perspective, it seems obvious that known EDCs must be banned entirely, with evidence provided that new chemicals are proven safe before they come to market rather than vice versa.
Can’t believe this is the first article I’ve come across (not that I was even looking for any) since I completed a double dissertation on EDs seventeen years ago as a University student. It reminded me of how passionate I was at the time and the struggle to explain it to most people because there was so little research around. It would solve many problems if quicker action could be taken at removing EDs from our environments. Great to see some published information about this.
It is definitely an opportunity for the wellbeing industry, one that other industries are better positioned to address. However, wellbeing is better positioned to identify the symptoms of the EDCs by paying attention to emotional and behavioral patterns. At U4Ea, we use emotions as symptoms, thus identifying which part of the endocrine system might be overactive.
Extremely important article. Thank you for printing it.
I am so happy to see this article as what you don’t know CAN KILL YOU..not to sound dramatic..just real! There are so many chemicals bombarding us every day and our homes may be the biggest culprits because of what we are using on and around our bodies. THis past year we have spent even more time at home increasing exposure. The good news is, we have choices in our home environment, even though not as much outside our home. Both effect us physically, mentally and emotionally..
When you know better you do better..so thank you Global Wellness Summit for raising awareness on a very important topic.
This is a very important subject, one that is spoken about in food, household and fashion industry but not yet in wellbeing where the subject should be placed as a priority. As the effects are so long term it can easily go under the radar or be ignored.
Do you know if there is any accessible long term studies available to read on ESG’s in skincare and wellbeing products? Or, is there a list of the most dangerous ESGs that our industry should be looking out for and questioning when procurement choices?